At University of California, population health means advancing the health and well-being of defined groups — whether communities, demographic populations, or patient cohorts — by understanding health outcomes, trends, and the social and clinical drivers behind them. Our work aims to improve care experiences and outcomes, reduce health care costs, and promote equitable health for all Californians and beyond.
What We Do
Our work in population health to further the delivery of value-based care across UC's health locations harnesses the strengths of our expert clinicians, researchers, data scientists and care teams to build systemwide approaches that are efficient, evidence-based and centered on the whole person. We use data and real-world insights to guide strategies that address not only disease, but the factors influencing health in everyday life.
Our mission is simple: help patients get the right care, at the right time, in the right place. This means improving patient knowledge, refining care coordination, reducing barriers to access and ensuring that treatment reflects individual needs and preferences.
Three core concepts guide our work to help people manage and improve their health.

Population health
Understanding and improving health and health outcomes of defined groups of people, which requires understanding and addressing the characteristics, disease burden and social drivers affecting their health.

Value-based care
Advancing models of care delivery that innovate to provide whole person care, which integrates services to address a person’s physical, mental, behavioral and social needs and conditions, while paying close attention to cost and access to care.

Social drivers of health
Addressing aspects of patients’ environments that may influence their overall health and well-being, with attention to identifying and intervening on health-related social needs.
Key initiatives driving impact
Systemwide initiatives in population health are focused on pressing health needs and innovative care solutions. Each initiative reflects UC’s commitment in health to evidence, collaboration and measurable impact.
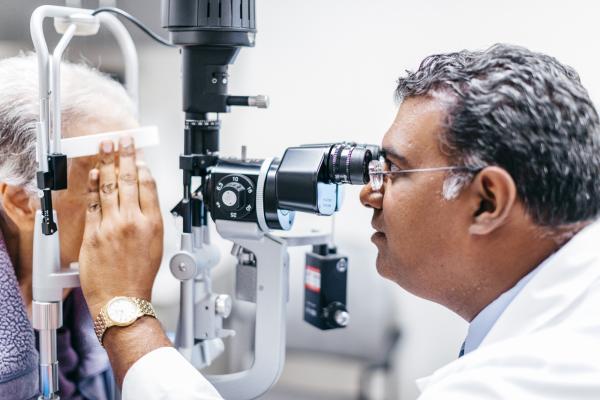
UC Health teams are working to make chronic disease management easier for patients. The Diabetes Care Management Initiative, led by UC Population Health, helps to integrate testing protocols, like blood glucose testing and eye examinations, into regular primary care visits. By including these screenings in routine primary care clinic visits, patients are able to take less trips and experience more integrated, team-based care.
UC is breaking down barriers to better diabetes care
UC teams are working to make chronic disease management easier for patients. The population health initiative on diabetes care management helps to integrate testing protocols, like blood glucose testing and eye examinations, into regular primary care visits. By including these screenings in routine primary care clinic visits, patients are able to take less trips and experience more integrated, team-based care.

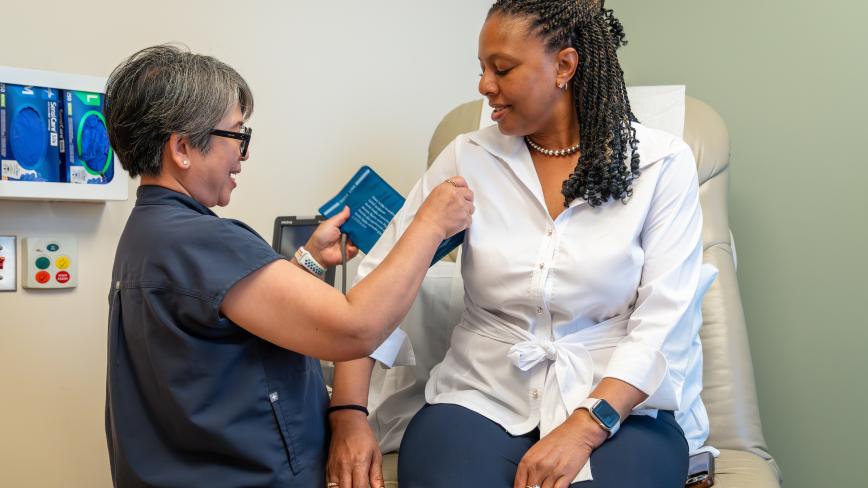
How putting pharmacists at the center is benefiting patients
Patients can face fragmented, confusing journeys as they deal with appointments, specialists, and medications, especially when a chronic or complex condition is present. Pharmacists are stepping in as crucial members of the care team, helping bring clarity, coordination and continuity to what can otherwise feel like an overwhelming process.

Using data to inform patient care
As an organization with a long history of innovation, University of California's researchers and clinical teams rely on data to help answer today’s most pressing health questions.
Reporting on our progress
Population health work across UC's hospitals and clinics focuses on advancing a vision of making care more impactful, effective and equitable for all the people we serve. More details about the data-driven systemwide initiatives that are advancing value-based care delivery, improving patient outcomes and optimizing resource use and costs are available in our annual population health report.

