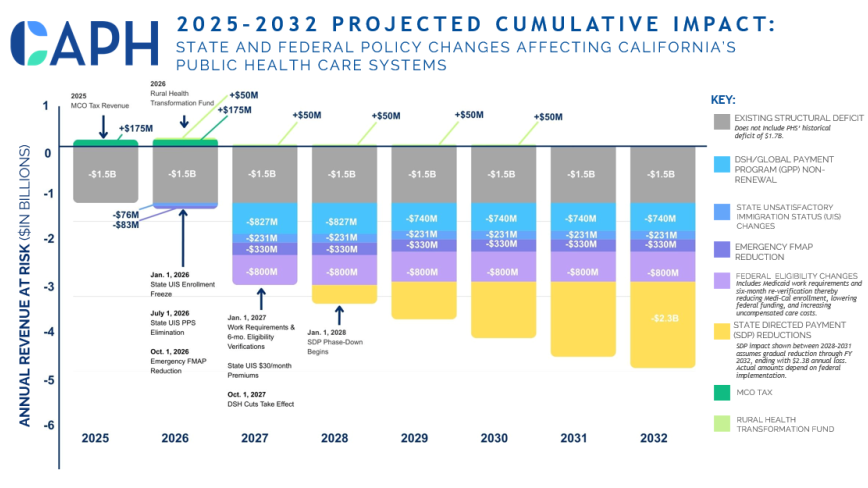
Two realities stand out as a result of federal H.R. 1 legislation: fewer Californians will have coverage, and the health care organizations that care for the state’s most vulnerable residents are already financially fragile.
H.R. 1 provisions will cause a ripple effect across the state, impacting people in need of care, regardless of insurance coverage.
Hospital systems have been innovating to adapt even before H.R. 1, but ongoing success depends on sustained state funding and support.
At a recent legislative and policy briefing hosted by University of California Health and California Association of Public Hospitals and Health Systems (CAPH), a panel of experts warned that federal actions would destabilize California’s statewide health care ecosystem that is already under strain.
These heightened concerns are driven by the provisions of H.R. 1—a federal budget and policy bill passed last summer that pays for tax cuts by narrowing Medicaid (Medi-Cal in California) eligibility and cutting funding for the program by roughly one trillion dollars nationally over the next decade.
“This is…an existential issue for safety-net providers,” said UC Health Executive Vice President David Rubin, M.D., who moderated the discussion.
Health care safety net system already on the edge
Public hospital systems, including UC’s academic health centers, which are part of California’s safety net, operate on persistently low reimbursement rates that fail to cover the cost of care for Medi-Cal members. Even before the federal changes, many organizations struggled to maintain services.
“The reality of public hospital systems and safety-net hospitals closing is here,” Rubin said.
Panelists for the event were UC Davis Health Interim CEO Michael Condrin, M.B.A.; Natividad CEO Chad Harris, M.D.; and CAPH President and CEO Erica Murray. They agreed that H.R. 1 compounds this fragility by simultaneously reducing coverage and cutting funding.
Medi-Cal coverage losses will drive more severe health conditions, more expensive care
By adding new bureaucratic barriers for Medi-Cal enrollees, including work requirements and more frequent eligibility checks, H.R. 1 will leave more Californians uninsured. But as panelists stressed, losing coverage does not eliminate the need for care. It just delays care, often with dangerous consequences.
“The first [priority] is to keep as many people covered in Medi-Cal as possible—full stop,” Murray emphasized.
Without coverage, patients are far less likely to access preventive and routine care. Instead, they delay treatment until conditions worsen, often dramatically.
“It’s not as if the patients go away,” Rubin said. “They just show up…with stage four disease.”
Natividad’s Harris illustrated this progression with a common scenario:
“You have a patient [who's] been well controlled on their diabetes medicine, insulin, or whatever the physician has decided. Now, they don't have access – or they're scared to come in – and [their blood] sugars are getting out of control. They show up in our emergency departments with an infection in their toe or some other part of their body. ...That’s gangrene. …That leads to things like infections in blood, sepsis, ICU visits. That person … has now ended up having an amputation or some other problem.”
“Patients are not going to have access to primary and routine specialty care…they’re going to come to us sicker,” Condrin said.
Then, emergency departments become the default point of care for unmanaged chronic illness and advanced disease that could have been better helped through early intervention in primary or specialty settings.
Medi-Cal changes will have a ripple effect across the state
The impact of changes from H.R. 1 will affect all Californians, not just Medi-Cal members, as California’s emergency departments are already stretched to capacity.
“We’re very concerned about…program closures and worse, hospital closure,” Condrin said.
He noted that as smaller public, rural and safety-net hospitals face financial collapse or service line reductions, patients will be funneled into fewer remaining points of care, further straining hospitals and medical centers such as UC Davis Health and causing delays in care.
Innovation in Medi-Cal is helping—but not enough without support
Hospital systems have been doing their part to address issues with Medi-Cal reimbursements and overcrowding even before H.R. 1. Panelists pointed to innovations under CalAIM as proof that targeted investments can improve outcomes and reduce costs.
At Natividad, leaders are preparing for coverage losses by restarting Esperanza Care, a program designed to serve uninsured residents, including farm workers who may lose Medi-Cal eligibility. The program aims to provide access to primary and specialty care for those who would otherwise fall through the cracks.
At UC Davis Health, a street medicine and care coordination initiative launched in partnership with Sacramento County brings care directly to patients in encampments and community settings, creating consistent access points outside of traditional clinics. Building on this, the system introduced a program focused on the highest users of emergency care, following 60 patients with frequent emergency department and inpatient visits.
“One of the very first patients…had been to the emergency department 33 times in 90 days…after intervention—not one visit,” said Condrin.
Through coordinated support—including community health workers, housing stabilization, field-based follow-up, and connection to primary care—the program demonstrates how addressing underlying needs can significantly reduce avoidable emergency department use.
Yet these successes depend on sustained state funding, as Condrin noted.
Looking ahead to the future of Medi-Cal
The briefing made clear that California's health care safety net ecosystem is approaching a tipping point. The question is not whether care will be delivered.
As Rubin said, “We will still care for [patients]... we will still meet our duty.”
Rather, health systems and state policymakers must examine how, where and at what cost as they work together to preserve coverage and stabilize funding.
About University of California Health
University of California Health comprises six academic health centers, 21 health professional schools, a Global Health Institute and systemwide services that improve the health of patients and the University’s students, faculty and employees. All of UC’s hospitals are ranked among the best in California and its medical schools and health professional schools are nationally ranked in their respective areas.
Editor’s note:
Erica Murray was the president and CEO of California Association of Public Hospitals and Health Systems at the time of the briefing. She became the associate vice president of strategic partnerships at UC Health on April 20, 2026.
Speakers’ quotations from the briefing event have been edited for clarity.